Recoupment has started or will soon begin for Medicare Part A and Part B providers and suppliers who received funds in 2020 under the Medicare Accelerated and Advance Payment (AAP) Program. The Centers for Medicare & Medicaid Services (CMS) provided $106 billion in AAP funding to alleviate the financial cash-flow burdens healthcare providers faced in the early stages of the 2019 novel coronavirus (COVID-19) pandemic. CMS began the COVID-19-related AAP funding with an announcement on March 28, 2020, and effectively ended funding by the end of April 2020. AAP recipients will now repay these funds through automatic recoupment from Medicare reimbursement.
As further background, CMS expanded its standard AAP process due to COVID-19 to provide additional liquidity to a larger group of providers and suppliers than typically would utilize the program. CMS announced the expanded AAP program with the expectation that automatic recoupment from reduced Medicare fee-for-service payments would begin 120 days after funding last summer. As the pandemic continued, CMS and its Medicare Administrative Contractors (MACs) generally did not begin to recoup AAP funds as scheduled. Congress then extended the period before recoupment so it would begin a full year after the date the individual provider or supplier received an AAP in the Continuing Appropriations Act, 2021 and Other Extensions Act, signed by President Trump on Oct. 1, 2020, as discussed in a Sept. 30, 2020, client alert. This legislation also extended the repayment timelines for the AAP program from 90 days (for most providers and suppliers) to 17 months, with reduced recoupment payments during this extended schedule, as discussed further below.
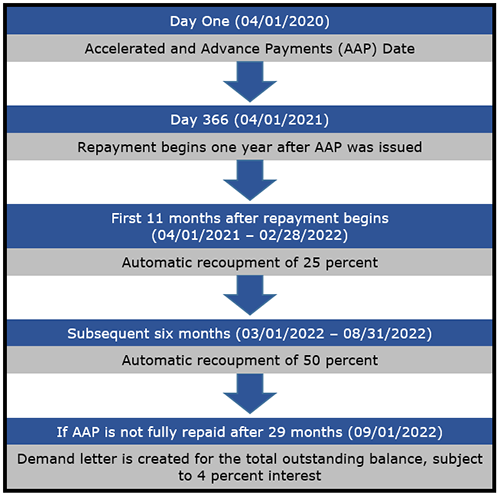
As recoupment begins, here are five key points recipients of AAP funds should understand about this process:
|
CGS Administrators, LLC (CGS) - Jurisdiction 15 First Coast Service Options Inc. (FCSO) - Jurisdiction N National Government Services (NGS) - Jurisdiction 6 & Jurisdiction K Novitas Solutions, Inc. - Jurisdiction H & Jurisdiction L Noridian Healthcare Solutions - Jurisdiction E & Jurisdiction F Palmetto GBA - Jurisdiction J & Jurisdiction M Wisconsin Physician Services (WPS) - Jurisdiction 5 & Jurisdiction 8 Noridian Healthcare Solutions, LLC – DME A & D CGS Administrators, LLC – DME B & C |
As the first AAP payments were made in March or April 2020, many providers and suppliers are quickly approaching the one-year anniversary of receiving an AAP. While the recoupment begins automatically with no action required by the provider or supplier, not all MACs are issuing reminder statements or notifications, relying on the CMS-issued MLN Matters article referenced above. Therefore, it is in the provider or supplier’s best interest to review its AAP application and history of accounting so there are no surprises once automatic recoupment begins. Further, providers and suppliers should notify their billing and financial staff that recovery will begin so they are not surprised with smaller payments. Some providers or suppliers’ recordkeeping systems may need to be reviewed to ensure this reduced payment amount does not create automatic system alerts. As mentioned above, a hotline is available for each MAC, if the provider has further questions after such reviews.
McGuireWoods is continuously monitoring information released by Congress and the Biden administration regarding COVID-19 and current legislation. Please contact the authors or any of the McGuireWoods COVID-19 Response Team members for additional information on the accelerated and advance payment programs and additional CARES Act funding and their availability to healthcare providers.